Healthy Aging Physical Therapy Monthly Blog
From Diagnosis to Late Stage Parkinson’s Disease: How Therapy for Parkinson’s Changes Over Time
Understand the stages of Parkinson’s disease and how therapy goals change over time. Learn how exercise, physical therapy, and proactive care can help you stay active, safe, and independent at every stage.
By: Dr. Katie Wadland, PT, DPT, Board-Certified Geriatric Clinical Specialist and Owner of Healthy Aging Physical Therapy
Parkinson’s disease is a progressive neurological condition that affects movement, balance, coordination, and overall function. While it is considered “progressive,” it’s important to recognize that this progression often occurs gradually—over many years, and in some cases, decades.
At Healthy Aging Physical Therapy, we understand that as the disease evolves, therapy should evolve with it. Our goal is to help our patients with Parkinson’s stay active, healthy, and safe at every stage of their journey.
In this blog, we’ll walk through the different stages of Parkinson’s disease and how therapy goals and approaches change over time to best support those evolving needs.
How Do We Define the Stages of Parkinson’s?
Clinically, Parkinson’s is often categorized using the Hoehn and Yahr Scale, which ranges from mild symptoms on one side of the body to more advanced mobility limitations.
In Stage 1, symptoms are mild and typically affect only one side of the body, often without significant impact on daily function.
In Stage 2, symptoms become more noticeable on both sides of the body, but balance is still largely intact and individuals remain independent.
In Stage 3, balance begins to decline, and fall risk increases, though individuals are usually still able to walk and perform many daily activities independently.
In Stage 4, symptoms are more advanced, and assistance is often needed for mobility and daily tasks.
In Stage 5, individuals may require a wheelchair or significant assistance with mobility and self-care.
But in real life, what matters most isn’t the number - it’s how symptoms are impacting daily movement and function. For that reason, we often think more practically in terms of early, middle, and later stages, with therapy evolving alongside those changes.
Early Stage Parkinson’s: Building the Foundation
In the early stages of Parkinson’s, changes are often subtle. Someone may notice a slight shift in posture, a reduced arm swing on one side, or that movements feel smaller or slower than they used to. Many people are still fully independent and may not feel like they “need” therapy yet.
In reality, there are some incredibly powerful things you can do early on that can help slow the progression of the disease and set you up to live well with Parkinson’s long-term—and therapy plays a key role in that education and guidance.
The focus during this stage is on building a strong foundation through exercise and movement awareness. Establishing a regular walking program is often one of the first steps, and this is something that should become part of your daily routine. Aerobic exercise is especially important, with the goal of gradually building up to 150–300 minutes per week of moderately intense activity. This level of exercise has some of the strongest evidence behind it as an effective way to help slow the progression of symptoms while also supporting overall health.
Strength training is another essential component, ideally performed two to three times per week. While strength training is important for all adults, it becomes even more critical for someone with a neuromuscular condition like Parkinson’s, where maintaining strength is key to preserving function and independence. Working with a physical or occupational therapist can help identify subtle asymmetries or early impairments—such as reduced shoulder mobility, postural changes, or decreased trunk rotation—that may not yet be limiting, but can become more impactful over time if not addressed. The benefit is that these findings can often be seamlessly incorporated into a well-rounded weekly routine that includes strength, mobility, and flexibility work.
This is also the stage when individuals are introduced to amplitude-based exercise programs, such as BIG, LOUD, or PWR! Moves. These programs focus on training larger, more intentional movements and are especially effective in Parkinson’s because they help counteract the tendency toward smaller, slower movement patterns. Starting these programs early—and continuing them consistently over time—can play a major role in maintaining your ability to move well.
At this stage, the overall goal is simple but powerful: use exercise strategically to stay ahead of the disease, rather than reacting to it later.
Middle Stage Parkinson’s: Maintaining Independence and Preventing Falls
As Parkinson’s progresses, changes become more noticeable and begin to impact daily life. Balance may feel less steady, walking may become more effortful, and challenges like freezing of gait—especially during turning or in tight spaces—can start to appear. This is often the stage when individuals first seek therapy after a fall or a noticeable decline.
At this point, the goal shifts from building capacity to maintaining independence and reducing risk.
Exercise remains a critically important part of disease management. Continuing a regular walking program is essential, though some individuals may benefit from introducing an assistive device to improve safety and efficiency. Aerobic exercise is still recommended in the 150–300 minutes per week range, but there is often a shift toward lower-risk options—such as a recumbent bike, elliptical, or NuStep—to allow for safer and more sustainable participation.
Strength training continues to play a key role, but therapy becomes more individualized and problem-focused. A physical or occupational therapist can develop a personalized balance program, address changes in gait, and help with fine motor challenges and difficulties with self-care and daily activities. Therapy at this stage also becomes increasingly focused on teaching you how to work with your body instead of against it. Simple but powerful strategies—like using external cues to improve walking—can make the difference between staying active and gradually reducing activity levels, which is something we work hard to prevent.
This is also the stage where new skills become essential—learning how to safely get up from the floor, how to manage freezing episodes, and how to navigate more complex movement challenges in daily life.
In addition, care often expands to include a broader team. Physical therapy, occupational therapy, and speech therapy may all play a role in addressing Parkinson’s-related changes, from rigidity and dyskinesia to fine motor challenges, voice changes, and swallowing difficulties.
Throughout all of this, amplitude-based programs like PWR! continue to serve as an important anchor, helping reinforce movement quality, confidence, and consistency.
At this stage, therapy becomes more about adapting, problem-solving, and preserving independence for as long as possible.
Later Stage Parkinson’s: Supporting Safety, Comfort, and Quality of Life
In the later stages of Parkinson’s, mobility becomes more limited and individuals often require increased support. Walking may become more difficult or less consistent, and caregivers frequently take on a larger role in daily care.
Even at this stage, therapy remains incredibly valuable—but the focus shifts again.
The goal is no longer just independence, but rather maximizing safety, comfort, and quality of life.
Movement is still encouraged, including walking as able, but often with modifications such as updated assistive devices or the introduction of wheeled mobility to improve safety and reduce fatigue. Aerobic activity remains important, though it is typically adapted to lower-risk formats that allow for continued participation without unnecessary strain.
Strength training continues as well, but often becomes more functional in nature—focusing on tasks like sit-to-stands, bed mobility, and transfers rather than traditional exercise formats.
A significant component of therapy at this stage involves supporting the environment and the caregiving team. This may include home modifications, equipment recommendations, and hands-on caregiver training to ensure safety with mobility and daily tasks.
Therapists also play a key role in minimizing secondary complications, such as contractures, skin breakdown, pain, and aspiration risk, while helping individuals maintain as much comfort and dignity as possible.
Even here, amplitude-based movement strategies can still be incorporated in a modified way to support engagement and movement quality.
At this stage, therapy is deeply focused on support, preservation, and quality of life—for both the individual and their caregivers.
The Common Thread Across Every Stage
While the goals of therapy evolve, a few principles remain constant.
Exercise continues to be one of the most powerful tools we have. Consistency matters. And perhaps most importantly, earlier and ongoing intervention leads to better outcomes.
Too often, therapy is only introduced after a fall or a hospitalization. But Parkinson’s is a lifelong condition—and care should evolve along with it, not stop and start during times of crisis.
Parkinsonisms: What Parkinson’s Is… and What It Isn’t
Learn the key differences between Parkinson’s disease and atypical Parkinsonism syndromes like PSP, MSA, Lewy Body Dementia, and CBD—and how diagnosis and rehabilitation approaches differ.
Written by: Dr. Katie Wadland, PT, DPT, Board-Certified Geriatric Clinical Specialist, Owner of Healthy Aging PT
When most people hear “Parkinson’s disease,” they picture a very specific condition—and for many, that’s accurate. But in our work at Healthy Aging Physical Therapy, we often meet patients whose symptoms look like Parkinson’s… but don’t quite follow the same rules.
These are called Atypical Parkinsonism syndromes, or simply Parkinsonisms.
As a Parkinson’s specialty practice, we’ve had the unique opportunity to work closely with individuals living with conditions like Lewy Body Dementia (LBD), Progressive Supranuclear Palsy (PSP), Multiple System Atrophy (MSA) and Corticobasilar Degernation (CBD). These diagnoses are less common - but incredibly important to recognize, as while there is overlap with Parkinson’s disease, the rehabilitation approach must be thoughtfully adapted for each condition.
Let’s break it down.
What Are “Parkinsonisms”?
“Parkinsonism” is a term used to describe a group of neurological conditions that share key movement features seen in Parkinson’s disease, such as:
Slowness of movement (bradykinesia)
Stiffness (rigidity)
Balance and gait difficulties
However, these conditions have different underlying causes, faster progression, and often respond differently (or poorly) to typical Parkinson’s medications like levodopa.
How Are Parkinsonisms Diagnosed?
Diagnosis can be challenging and often evolves over time. Often, someone is initially diagnosed with Parkinson’s Disease, but when symptom progression is different than expected, or the individual does not respond to medications as expected, an atypical form may be suspected. Other signs might include:
Early balance impairment or falls
Cognitive or autonomic changes early in the disease course
Eye movement abnormalities (especially in PSP)
Imaging and neurological exam findings
In many cases, diagnosis is clinical and may take time, as symptoms unfold and patterns become clearer. Fortunately, we now have more concrete ways to differentiate between the different syndromes including DAT Scans and Skin Biopsies:
DAT Scans: A DaTscan is a specialized imaging test that looks at dopamine activity in the brain. By looking at the patterns, doctors can now better identify if symptoms are coming from a neurodegenerative cause, like Parkinson’s Disease or an Atypical Parkinson’s Syndrome, or from something else, like Essential Tremor or drug-induced symptoms. It is important to be aware a DAT Scan can NOT differentiate between idiopathic Parkinson’s and Atypical Parkinson’s Disease.
Skin Biopsies: A skin biopsy can be taken and analyzed for abnormal alpha-synuculein deposits. When these are identified in the sample, it can help differentiate between the idiopathic form of Parkinson’s and some of the atypical forms of the disease. It is important to note that while it can differentiate the two from one another, it can NOT identify which Atypical Parkinson’s disease a person may have.
As you can see, while we have many more tools at our disposal for proper diagnosis of Parkinson’s Disease and Atypical Parkinsonisms, it still remains a largely clinical diagnosis based on symptoms, progression of disease and response to medication treatment.
What are the Different Atypical Parkinson’s Diseases?
Lewy body Dementia (LBD)
Lewy Body Dementia is a neurodegenerative condition characterized by a combination of:
Cognitive impairment
Parkinsonian motor symptoms
Fluctuations in alertness
Visual hallucinations
What Makes It Different Than Parkinson’s?
Cognition is affected early, often before or alongside movement symptoms
Fluctuating attention and alertness (good days and bad days are common - and presentation may even within throughout the day)
Visual hallucinations are common
Patients may be sensitive to certain medications
How Is Rehab Different?
Rehabilitation for LBD requires a flexible, patient-centered approach:
Session-to-session variability is expected. Therapists must be prepared to adjust treatments, as needed, in real time.
Patients do best when care is focused on routine, familiarity, and caregiver involvement.
Due to the cognitive challenges, communication should be clear, calm and simple.
Balance and mobility training are still essential, but, patients may may need shorter sessions or breaks and should focus should focus more on compensatory strategies as it will be harder for patients to carryover instructions from session to session.
Progressive Supranuclear Palsy (PSP)
PSP is a neurodegenerative condition that affects:
Balance and walking
Eye movements (especially looking down)
Postural control (and most notably, results in retropulsion, or the sensation of falling backwards)
Spinal mobility (rigidity is a marked feature in people with PSP)
What Makes It Different Than Parkinson’s?
Early and frequent falls, often backward
Difficulty with vertical eye movements, especially downward gaze
Speech and swallowing issues tend to appear earlier
Minimal response to Parkinson’s medications
Axial rigidity (stiffness in the trunk more than limbs)
How Is Rehab Different?
Rehabilitation for PSP is very focused on safety and proactive management of symptoms:
Fall prevention is a #1 priority. This often involves prescribing an appropriate assistive device (we love the USTEP for our patients with PSP!), making changes to the home to make it safer and making recommendations for adequate supervision and teaching caregivers the skills they need to help their loved one move safely.
Therapists should assess and treat ocular coordination impairments. When patients can’t look down well, this impacts depth perception and fields of vision, making things like using stairs, curbs and navigating uneven terrain more difficult. People with PSP benefit from working on compensatory skills like visual scanning, and also on using visual exercises to maintain the ocular control they have.
Because of the areas impacted by PSP, people with PSP will have a more difficult time improving balance reactions and walking. They frequently do better with use of external cuing, like using targets on the floor or a laser, or by putting signs up throughout the home to remind them to use safe strategies like pushing off the chair to stand up, or holding on to a surface for support before reaching for something.
It is critical for someone with PSP to get therapy early! Progression of PSP is faster than in typical Parkinson’s Disease and the earlier we can address emerging changes and new symptoms, the more impact we can have on safety and quality of life.
Multiple Systems Atrophy (MSA)
MSA is a progressive neurological condition that affects:
Movement (Parkinsonian features)
Posture (more rounded, head-down positions)
Autonomic Nervous System (causing changes in blood pressure, bladder control and breathing)
What Makes It Different Than Parkinson’s?
Significant autonomic dysfunction causing frequent low blood pressure and syncope (passing out)
Bowel and bladder dysfunction is more common
Progression is faster than in typical Parkinson’s Disease
Minimal response to Parkinson’s medications
May also include cerebellar features like coordination issues
How Is Rehab Different?
Rehabilitation for MSA is requires careful monitoring and management of blood pressure in particular:
Vital sign monitoring should be completed before and during sessions and sessions may need to be modified to keep blood pressure in safe ranges.
Education should focus on strategies to maintain blood pressure in safe ranges throughout the day. This often requires a combination of medication management and coordination with doctors, and education for the patient and caregivers for using things like compression stockings or abdominal binders to help keep blood pressure high enough when they stand up.
Because orthostatic hypotension is common in MSA (drops in blood pressure with standing), it is important to include a seated warm up and slow progression to standing and walking activities during sessions.
Hydration is critical for patients with MSA. Being dehydrated will make the autonomic dysregulation worse and is a frequent cause of falls and hospitalizations for these patients.
Corticobasilar Degeneration (CBD)
CBD Corticobasal Degeneration (CBD) is a rare neurodegenerative condition that affects both the cortex (brain) and the basal ganglia, leading to a combination of movement and higher-level motor planning difficulties. It often presents asymmetrically, meaning one side of the body is significantly more affected than the other.
What Makes It Different Than Parkinson’s?
CBD has several unique features that sets it apart:
Marked asymmetry with one side affected more than the other
Apraxia is a key feature, which is difficulty performing purposeful or functional movements with a limb despite having the strength and motor control to do so
‘Alien Limb’ phenomenon is common - an arm or leg may seem to move involuntarily or feel disconnected from the body
Cortical sensory deficits make it difficult to interpret sensory information
Myoclonus is often present which looks like jerky or uncontrolled movements
Minimal to no response to Parkinson’s medications
Unlike Parkinson’s disease, where movement is primarily limited by slowness and rigidity, CBD involves a breakdown in motor planning and control at a higher neurological level.
How Is Rehab Different?
Rehabilitation for CBD Rehabilitation for CBD requires a shift in approach from “strength and movement” to motor planning, task breakdown, and functional adaptation:
Therapy should focus on task-specific training, and patients do best when breaking down movements into smaller, step-by-step components
Cuing should incorporate external cues, hand-over-hand support and modeling or demonstration as interpretation of body-based or sensory-cues will be very hard to understand
Compensation with the less affected side is critical to maintaining independence as long as possible
Consider use of adaptive strategies and equipment early on so training can be incorporated while motor control and cognition is at it’s best.
The Big Picture: Similar…But Not the Same
While all Parkinsonisms share common movement challenges, the differences between them matter—a lot. In Parkinson’s disease, we typically see a slower progression, a good response to medication (especially early on), and a rehabilitation approach that emphasizes amplitude, intensity, and long-term maintenance. In contrast, atypical Parkinsonisms often present with a faster or more complex progression and a more limited response to medication. Because of this, rehabilitation must shift—becoming more adaptive, more preventative, more caregiver-inclusive, and more medically integrated to address the broader range of symptoms these conditions can bring.
Hopefully this information has helped you better understand some of the key differences between typical, or idiopathic, Parkinson’s disease and the atypical forms of Parkinsonism. Whether you are a patient, caregiver, or therapist reading this, it is critical to recognize these differences—not only to advocate for an accurate diagnosis if things “just don’t feel right,” but also to find providers who understand these conditions and can truly individualize care.
OneStep Closer: Making Sense of your OneStep Data
Learn what your OneStep gait data means and how walking speed, step symmetry, cadence, and Walk Score help reduce fall risk and improve balance in older adults.
Written by: Dr. Katie Wadland, PT, DPT, Board-Certified Geriatric Clinical Specialist and owner of Healthy Aging Physical Therapy
Last month, we introduced OneStep, the walking and movement app we now use at Healthy Aging Physical Therapy to better understand how our patients move in the real world - at home, in the community and both with and without their therapists.
While we’ve been loving the experience of using OneStep so far — and many of you have enjoyed seeing your progress in real time — we’ve also received some great feedback: “What do all these numbers actually mean?”
So this month, we’re diving deeper. This blog — along with our social media posts throughout March — will focus on breaking down exactly what we’re measuring, what the data tells us, and why it matters for your safety, strength, and independence.
Let’s break down what we’re measuring—and why it’s so powerful.
Walking Is More Than Just Speed
Most people assume walking is simply about how fast you move from point A to point B. In reality, walking is a complex, whole-body activity that reflects strength, balance, coordination, confidence, and even cognitive load.
Using OneStep, we’re able to measure multiple aspects of your walking pattern over time, giving us a clearer picture of both current safety and future risk.
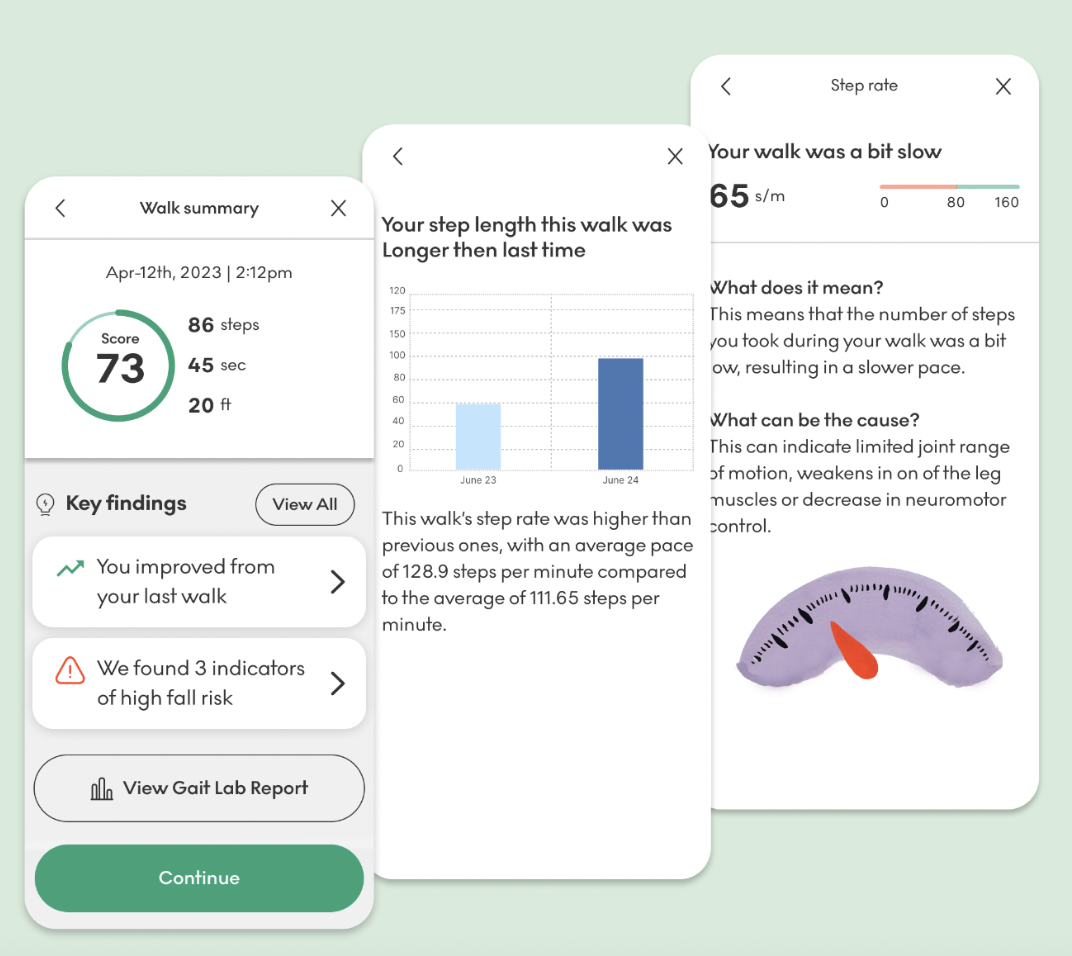
The Big Picture: Your Walk Score
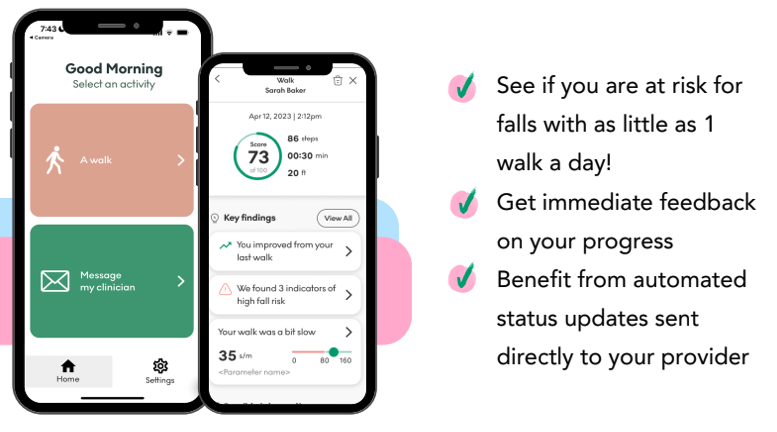
One of the first things you may notice in OneStep is your Walk Score.
This is a single number (out of 100) that summarizes how:
Steady your steps are
Consistent your rhythm is
Smoothly you move from step to step
A higher Walk Score reflects a safer, more efficient walking pattern. While we never rely on one number alone, this score helps us track meaningful changes over time and identify when something may need attention.
Understanding other Key Walking Parameters
Walking Speed (Velocity)
Walking speed is measured in meters per second and is one of the strongest indicators of functional mobility.
Slower speeds may reflect weakness, balance challenges, or reduced endurance
Inconsistent speed may signal fatigue, distraction, or instability
While 1.0–1.2 m/sec is typical for healthy adults, many of our patients do very well with a goal closer to 0.8 m/sec, which is strongly correlated with safe household mobility and independence.
Cadence (Steps per Minute)
Cadence is how many steps you take per minute while walking.
Very slow cadence can be linked to balance concerns, reduced confidence, or cautious movement
Very fast or uneven cadence can indicate rushing or difficulty controlling speed
For many adults, a steady cadence between 100–120 steps per minute is associated with comfortable, efficient walking. In Parkinson’s Disease, we often see cadence increase which is reflective of a ‘shuffled’ or ‘freezing’ gait - and something we are quickly finding can be significantly improved with this type of in-the-moment feedback.
Velocity Variability
This measures how consistent your walking speed is from step to step.
Low variability = steady, predictable walking
High variability = frequent changes in speed, often linked to balance challenges, fatigue, or environmental demands
Our general goal is less than 20% variability, reflecting controlled and confident movement.
Consistency
Consistency looks at how similar each step is to the next and is scored from 0–100.
Scores between 80–100 suggest a stable, repeatable walking pattern
Lower scores may reflect coordination changes, balance challenges, or neurologic conditions
This is an especially valuable number to monitor for patients with Parkinson’s disease, neurologic diagnoses, or anyone at risk for falls.
Looking Deeper: Step Symmetry, Timing, and Joint Motion
Beyond the general measures above, OneStep allows us to analyze more detailed gait data about spatial and temporal parameters, and joint range of motion, including:
Average step length
Step length asymmetry
Single-leg and double-leg support time
Stance symmetry
Step width
Hip and femoral range of motion during walking
These details help us identify why your walking may feel uneven, where balance is breaking down, and how strength, coordination, or joint immobility may be contributing - and this level of insight allows us to be more precise, and more effective, in your treatment.
Daily Step Count: Measuring Movement to Get You Moving More
Finally, OneStep also tracks your daily step count by connecting to your phone’s internal pedometer (and can sync with devices like Apple Watch or Fitbit).
Why this matters:
More daily steps are associated with better balance, strength, endurance, and overall health
Even small increases in daily walking can lead to meaningful improvements
For the most accurate data, we recommend carrying your phone in your pocket during as many walks as possible. Together, we’ll determine a personalized, safe daily step goal that you can work up to slowly, to promote optimal health and wellness as you age or live with chronic disease or disability.
Why This Matters at Healthy Aging Physical Therapy
At Healthy Aging Physical Therapy, our goal is not just to help you walk more, but to help you walk better, safer, and with more confidence.
By combining expert clinical care with real-world movement data, OneStep helps us:
Detect subtle changes earlier
Personalize care more precisely
Track progress that truly matters
Support long-term independence and fall prevention
We hope this blog post helps you better understand what you’re seeing in your OneStep data and feel more confident about how we’re using it to guide your care. This is what modern, whole-person physical therapy looks like - and we’re excited to take this journey with you.
Taking ‘OneStep’ Forward Towards Better Walking and Balance Outcomes
Healthy Aging Physical Therapy is excited to introduce OneStep in 2026 — an innovative smartphone-based tool that allows our clinicians to objectively measure gait, balance, and fall risk both in person and remotely. Learn why gait is considered the “sixth vital sign” and how OneStep helps us personalize care, track progress, and identify early signs of decline for older adults, people with Parkinson’s disease, orthopedic concerns, and balance or vestibular conditions.
Written By: Dr. Katie Wadland, PT, DPT, Owner: Healthy Aging Physical Therapy
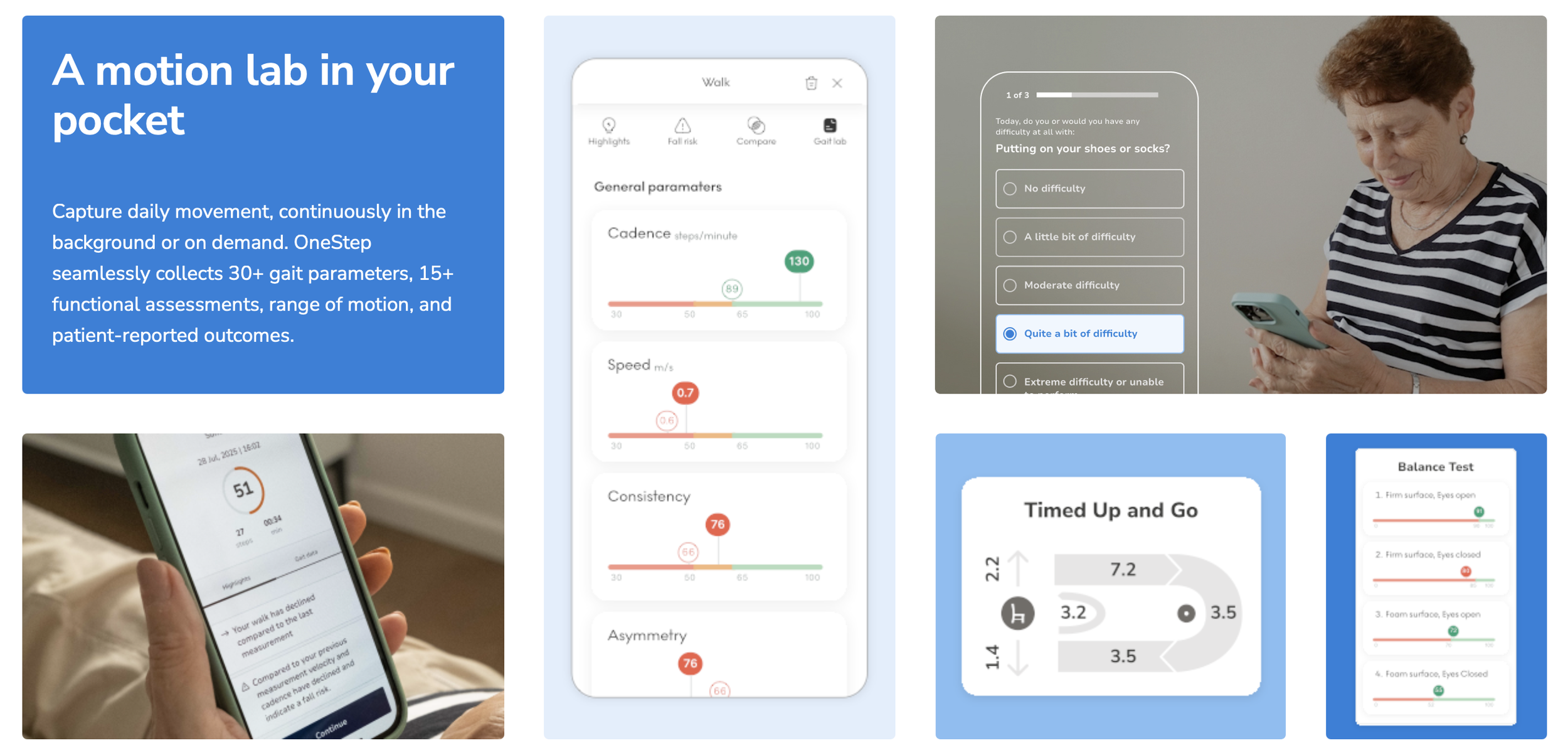
At Healthy Aging Physical Therapy, our mission is to deliver the most effective, evidence-based care available. That’s why we’re excited to introduce OneStep, a cutting-edge clinical gait analysis and remote monitoring platform we’ll begin offering to patients in February 2026. OneStep transforms a patient’s smartphone into a clinical-grade motion laboratory, allowing us to capture high-fidelity gait and mobility data both in clinic and in real-world environments using the device you already carry.
By simply putting a phone with our OneStep app in your pocket while you move around, we can:
Quantify walking speed, stride length, cadence, movement symmetry, variability, balance indicators, and other spatiotemporal gait metrics, all critical indicators of mobility and fall risk.
Detect fall risk and mobility decline earlier, enabling proactive adjustments to your care plan.
Monitor progress objectively and continuously throughout your plan of care - entirely remotely.
Improve patient engagement by showing concrete progress data rather than relying solely on subjective reports.
OneStep’s dashboard synthesizes movement into actionable clinical insights, helping your therapist tailor interventions based on quantitative evidence rather than estimation.
Evidence and Clinical Value
The scientific community increasingly recognizes gait, and particularly gait speed, as a key indicator of health. In fact, walking speed is referred to as the “sixth vital sign” because of its strong predictive value for functional decline, fall risk, future disability, hospitalization, and even longevity.
Beyond just “how fast” someone walks, gait characteristics reflect the integrated functioning of multiple physiological systems, including cardiovascular, neurological, and musculoskeletal health. Slower gait speed has been shown in multiple studies to correlate with increased risk of falls and adverse outcomes across older adult populations.
But Does it Work?
Peer-reviewed research has validated that smartphone-based gait analysis applications can provide reliable alternatives to traditional motion-laboratory measures and are feasible for evaluating gait dysfunction in clinical settings.
This supports our confidence that OneStep’s data is not just convenient, it is clinically meaningful and can augment traditional evaluation tools to give a fuller, real-world view of your mobility and fall risk.
Furthermore, OneStep’s own performance metrics (derived from aggregated real-world use) demonstrate its value:
The platform has analyzed tens of billions of steps and been used in mobility assessments for hundreds of thousands of patients, extracting 30+ gait and mobility parameters that clinicians rely on.
Organizational outcomes reported on OneStep’s platform include reductions in falls, improvements in patient engagement, and measurable time savings for clinicians, underscoring its operational as well as clinical impact.
Why This Matters to You
Traditional gait and balance assessments that we perform with you at home remain an essential part of your care. However, they are ultimately momentary snapshots of how you walk in that specific moment, often while your therapist is standing close by, observing, cueing, or providing supervision.
For many people, this setting does not fully reflect natural walking patterns. The presence of a clinician can unintentionally change how someone moves. Increased focus, heightened awareness, performance pressure, or a sense of being “watched” can lead to walking faster, more cautiously, or with more effort than usual. In some cases, people walk better than they typically do day to day; in others, they move more stiffly or guarded than normal.
As a result, what we see during a single assessment may not capture:
How you walk when you are relaxed and moving naturally
How fatigue, distraction, or multitasking affect your gait
How your walking changes throughout the day or across environments
Early signs of decline that emerge gradually rather than suddenly
By combining in-person clinical assessments with real-world gait monitoring, we gain a more complete and accurate picture of your mobility. This allows us to tailor your care not just to how you can walk when supervised, but to how you actually walk in daily life.
OneStep extends this model by providing:
Continuous monitoring across environments and times, capturing variations that might be missed in a single clinic visit.
Objective, quantifiable progress tracking instead of subjective impressions alone.
Early identification of decline or risk, allowing timely intervention before issues result in falls or functional loss.
This translates into more personalized care, more meaningful outcomes, and the ability to tailor interventions with precision.
Why Gait Matters for the Populations We Serve
While gait is a powerful health indicator across the lifespan, it is especially meaningful for the populations we work with every day. Subtle changes in walking patterns often appear before patients notice functional decline — and long before a fall, injury, or loss of independence occurs.
Older Adults
In older adults, gait speed, variability, and symmetry are strongly associated with:
Fall risk
Frailty progression
Loss of independence
Hospitalization and mortality risk
Even small reductions in gait speed (as little as 0.05–0.10 m/s) have been shown in research to represent clinically meaningful decline. Conversely, measurable improvements in gait speed correlate with improved survival and functional outcomes.
By tracking gait longitudinally, OneStep allows us to:
Identify early decline before it becomes a crisis
Distinguish “normal aging” from actionable impairment
Objectively measure improvement from strength, balance, and mobility interventions
Monitor mobility over time for patients on maintenance or wellness-based plans of care
For many older adults, gait truly reflects the intersection of strength, balance, endurance, cognition, and confidence.
Parkinson’s Disease and Other Neurologic Conditions
In Parkinson’s disease, gait is one of the most sensitive indicators of disease progression and functional impact. Changes in gait often include:
Reduced stride length
Shuffling or festination
Increased gait variability
Asymmetry
Freezing episodes
Reduced arm swing and trunk rotation
These changes can fluctuate day-to-day based on medication timing, fatigue, and environment — meaning they are often missed during brief clinic assessments.
With OneStep, we can:
Quantify changes in stride length, cadence, and variability over time
Monitor real-world walking, not just “best performance”
Identify subtle decline earlier and adjust interventions proactively
Better individualize cueing strategies, amplitude-based training, and balance work
Help monitor for changes in mobility related to medications, DBS and other therapies
This data supports more precise, responsive care, particularly for individuals living with Parkinson’s disease who benefit from long-term monitoring and early intervention.
Orthopedic Conditions
For patients with orthopedic concerns, including joint replacements, arthritis, spine conditions, or lower-extremity injuries, gait often compensates long before pain fully resolves.
Common gait-related issues include:
Asymmetrical loading
Reduced stance time on the involved limb
Altered cadence or step length
Persistent compensations that increase stress on other joints
OneStep allows us to:
Objectively assess symmetry and loading patterns
Track recovery beyond pain reduction alone
Ensure gait normalization, not just task completion
Identify lingering deficits that may increase reinjury risk
This helps ensure that “feeling better” also means moving better, reducing long-term wear and injury risk.
Balance and Vestibular Conditions
For patients with vestibular disorders or balance impairments, gait often reveals deficits that static balance tests do not.
Changes may include:
Increased gait variability
Slower walking speed
Widened base of support
Hesitancy or avoidance in real-world environments
Because balance confidence and sensory integration vary by environment, gait measured outside the clinic provides critical insight.
With OneStep, we can:
Assess dynamic balance during everyday walking
Monitor response to vestibular rehabilitation over time
Identify sway and movement during static balance assessments
Better tailor progression of dynamic balance and dual-task training
This allows us to move beyond symptom resolution toward true functional confidence and safety.
Want to Take ‘OneStep’ Closer to Better Walking and Balance With Us?
Beginning in February 2026, OneStep will be integrated into care at Healthy Aging Physical Therapy as part of our comprehensive assessment and treatment planning process.
During your evaluation or reassessment, your clinician may use OneStep to help measure and better understand your walking and balance. In some cases, we may ask you to download the OneStep app to your phone and use it as a way for us to track gait and mobility data over time during your plan of care - both in person and, when appropriate, remotely.
There is no additional cost to you for using OneStep during skilled physical therapy.
You can expect your clinician to:
Explain how OneStep works and how it uses your phone to measure walking
Review which gait and mobility metrics are relevant to your goals
Use this information to more precisely tailor your treatment plan and monitor progress or change over time
Interested in Gait Insights, but not a Current Patient?
If you’re interested in understanding your gait, balance, or fall risk, but are not in need of skilled physical therapy services, you may request a Wellness Evaluation through our Wellness365 Program. This allows you to experience OneStep, receive objective gait data, and gain professional insight into your movement patterns outside of an insurance-based plan of care. We will also be rolling a third tier in our Wellness365 program to allow for long term engagement with your therapist and ongoing monitoring of your gait, mobility and exercise program so stay tuned for more details!
Gait is more than movement - it is a vital signal of health. OneStep gives us a powerful, data-driven way to listen. If you have questions or would like to learn more, we’re happy to talk with you.